Hip Osteoarthritis
Hip osteoarthritis is a common cause of groin pain, stiffness and reduced confidence in walking, particularly in midlife and beyond. For some people, symptoms develop gradually over years. For others, they begin with intermittent flare-ups that become more frequent over time.
Although often described as “wear and tear,” hip osteoarthritis is a more adaptive and dynamic process than that phrase suggests. Structural changes occur within the joint, but pain is influenced by far more than cartilage alone. Muscle strength, load tolerance, joint mechanics, flare-related inflammation and nervous system sensitivity all contribute to how the hip feels on a daily basis.
At Solent Specialist Physiotherapy, we understand the broader picture, allowing treatment to focus on restoring movement and resilience rather than fearing structural damage.

What Actually Happens in Hip Osteoarthritis?
Hip osteoarthritis involves gradual changes in the cartilage, bone and joint lining. The body attempts to adapt to years of load and movement. Sometimes these adaptations lead to stiffness, reduced range of motion and activity-related pain.
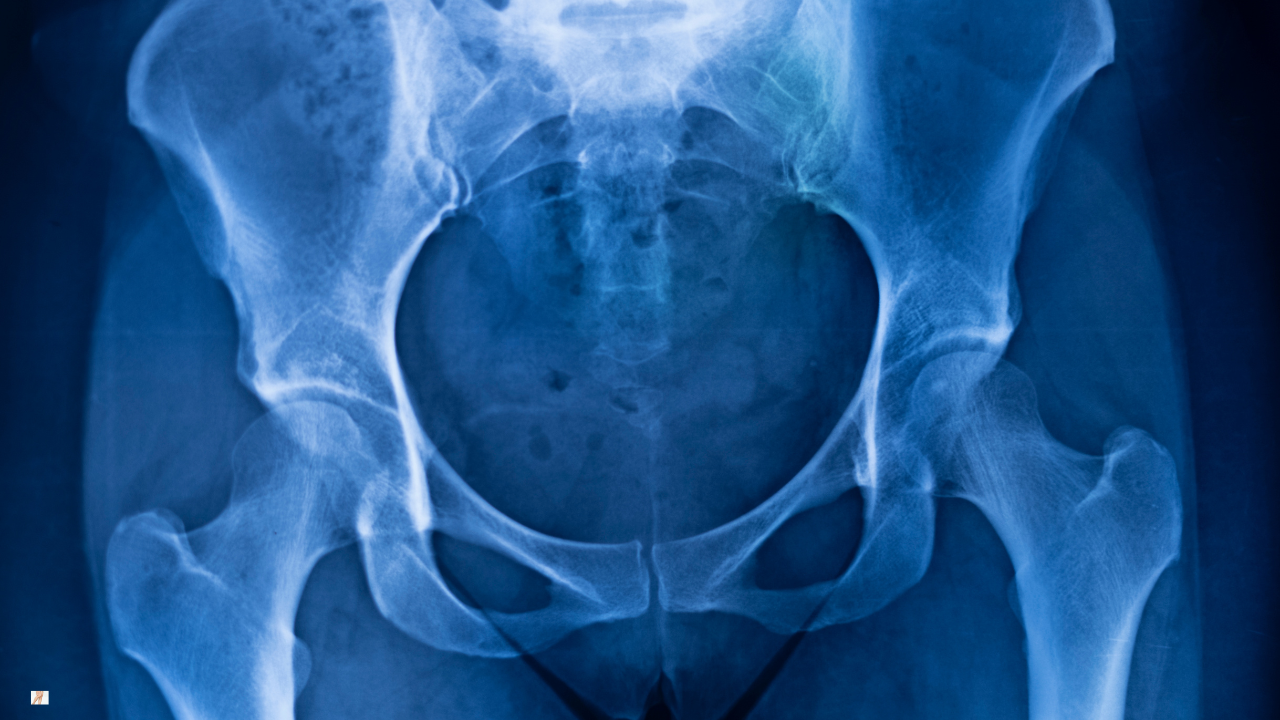
Imaging findings do not always reflect symptom severity. Many people show arthritic changes on X-ray yet function well. Others experience significant discomfort despite modest imaging changes. This is why treatment decisions should be based on symptoms and functional limitation — not imaging language alone.
How Hip Osteoarthritis Commonly Presents
Hip osteoarthritis often causes pain in the groin, front of the thigh or buttock. Some people notice discomfort turning in bed, putting on socks or shoes, getting in and out of a car, or walking longer distances. Stiffness in the morning or after sitting is common, usually easing within thirty minutes.
Flare-ups may occur following increased walking, hills, travel or changes in routine. During a flare, the hip may feel more painful, tight or irritable for several days or weeks. These episodes rarely indicate sudden deterioration. They more commonly reflect temporary increases in joint sensitivity.
Learning to manage flare-ups calmly and intelligently reduces fear and prevents prolonged setbacks.
Is Movement Damaging the Hip?
A common concern is that continued use of an arthritic hip will accelerate damage. In reality, appropriately graded activity supports joint health. Muscles surrounding the hip act as shock absorbers and stabilisers. When strength declines, joint load often increases.
Avoidance of movement can lead to reduced muscle support, increased stiffness and heightened sensitivity. Rehabilitation focuses on rebuilding hip strength, improving load tolerance and restoring confidence in everyday movement.
The aim is not to eliminate all discomfort immediately, but to improve function and long-term resilience.
Imaging: When Is It Helpful?
A clinical assessment is often sufficient to guide management. X-rays can confirm structural osteoarthritis but do not determine prognosis on their own. MRI is rarely required unless symptoms suggest another diagnosis.
Imaging may be useful when surgical options are being considered or when symptoms are atypical. However, the interpretation of imaging findings should always be balanced with clinical presentation.
Understanding what your scan does — and does not — mean is an important part of specialist care.
Managing Hip Osteoarthritis Flare-Ups
Flare-ups can feel unsettling, particularly when they interfere with sleep or walking. They often follow increases in load or prolonged activity.
During a flare, the goal is not strict rest but temporary modification. Reducing aggravating movements, maintaining gentle mobility, using appropriate pain relief if needed, and gradually reintroducing strengthening once symptoms settle can shorten recovery time.
Knowing that flare-ups are part of the condition — not a sign of failure — helps maintain confidence.
Injection Therapy for Hip Osteoarthritis
Injection therapy may provide symptom relief for some individuals, particularly when pain is limiting rehabilitation progress.
Corticosteroid injections can reduce inflammation temporarily. Other injection options may be discussed depending on clinical presentation.
Injections do not reverse structural changes. Their role is often to reduce pain sufficiently to allow strengthening and functional progress. If an injection provides meaningful relief, repeat treatment may be considered at appropriate intervals under specialist guidance.
Injection decisions should always form part of a broader management strategy rather than replace rehabilitation.
When Is Hip Replacement Appropriate?
Hip replacement surgery can provide excellent outcomes for carefully selected individuals when pain and function remain significantly impaired despite well-structured rehabilitation.
However, surgery is not inevitable. Many people manage hip osteoarthritis successfully for years with strengthening, load management and targeted guidance.
Shared decision-making is central. This involves discussing symptom severity, impact on quality of life, realistic expectations of surgery, recovery timelines and alternative options. A specialist assessment can help clarify whether continued conservative care or surgical referral is appropriate.
The decision should be informed, considered and aligned with your goals.
For individuals who proceed to joint replacement, structured rehabilitation remains essential. You can learn more about our specialist post total hip replacement rehabilitation service here→
Our Specialist Approach to Hip Osteoarthritis
Management is tailored to your stage of symptoms, lifestyle demands and long-term goals.
Treatment focuses on progressive strengthening of the hip musculature, improving load tolerance during walking and functional tasks, addressing movement patterns that may increase joint stress, and guiding flare management.
Where appropriate, we discuss injection therapy, referral pathways and long-term planning. The aim is to preserve independence, reduce pain and support confident movement.
Understanding Osteoarthritis
Hip osteoarthritis is one of several joint conditions within our specialist osteoarthritis service. If you would like to understand more about how osteoarthritis develops, why flare-ups occur, and how structured rehabilitation supports long-term joint health, you can read our overview on specialist physiotherapy for osteoarthritis.
Learn More About OsteoarthritisFrequently Asked Questions About Hip Osteoarthritis
Is groin pain always osteoarthritis?
Is walking good for hip arthritis?
Will strengthening make my hip worse?
Does hip osteoarthritis inevitably worsen?
Should I delay hip replacement?
Does “bone on bone” mean my knee is beyond help?
Book a Specialist Hip Assessment
If hip osteoarthritis is affecting your mobility, confidence or quality of life, appointments are available within our specialist clinics. Assessment focuses on restoring strength, managing flare-ups and guiding informed decisions about long-term care.
Appointments for hip osteoarthritis are available within our specialist clinic in Gosport.
Book Your Hip Assessment

